Imagine undergoing abdominal surgery through incisions no larger than a fingernail — recovering in days instead of weeks, and returning home the same day the procedure was performed. This is the everyday reality of laparoscopic surgery, one of the most transformative advances in modern medicine. Whether your doctor has recommended it or you are simply curious, this guide will walk you through everything you need to know.
What is laparoscopic surgery?
Laparoscopic surgery — also called minimally invasive surgery or keyhole surgery — is a modern surgical technique in which operations inside the abdomen or pelvis are performed through small incisions, typically between 0.5 and 1.5 centimetres in length. In contrast to traditional open surgery, which requires a large incision to directly access the organs, laparoscopic surgery uses a slender tube-like instrument called a laparoscope. This device is fitted with a high-resolution camera at its tip, projecting a magnified live image of the internal organs onto a monitor in the operating theatre.
The term itself comes from the Greek words lapara (flank or abdomen) and skopein (to examine). The first laparoscopic procedure was performed in the early twentieth century, but the technique only became widespread in the late 1980s when laparoscopic cholecystectomy — gallbladder removal — was successfully performed and quickly adopted as the gold standard for that surgery.
Key fact: Laparoscopic surgery does not mean no surgery. It still involves anaesthesia, incisions, and post-operative recovery — but all of these are significantly reduced compared to traditional open procedures.
How does the procedure work?
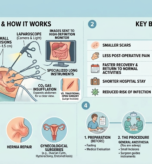
Understanding what happens in the operating theatre helps patients feel more confident and prepared. The process follows a carefully structured sequence:
- Anaesthesia:The patient is placed under general anaesthesia, ensuring complete unconsciousness and absence of pain throughout.
- Insufflation:Carbon dioxide gas is introduced into the abdominal cavity through a small needle. This inflates the abdomen like a dome, creating working space for the surgeon and keeping organs separated for better visibility.
- Trocar insertion:Small hollow tubes called trocars are inserted through the incisions. These act as ports through which the laparoscope and surgical instruments are passed.
- Visualisation:The camera transmits a real-time, high-definition image to screens in the theatre. Surgeons operate while watching this monitor rather than looking directly into the body.
- The operation:Using long, thin instruments passed through the trocars, the surgeon performs the procedure — cutting, stitching, removing tissue, or repairing structures as needed.
- Closure:Instruments are removed, CO₂ gas is released, and the small incisions are closed with sutures or skin glue.
Key benefits over open surgery
The advantages of Laparoscopic surgery over conventional open surgery are significant, which explains why surgeons and patients alike prefer it whenever it is technically feasible. Patients experience less post-operative pain because the muscle tissue is not cut open widely. Smaller incisions also mean a substantially lower risk of wound infection, reduced blood loss during the procedure, and minimal scarring that is largely invisible once healed.
Recovery is dramatically faster. Most laparoscopic patients return to light daily activities within a week and to full normal function within two to three weeks, compared to six to eight weeks for open surgery. Hospital stays are shorter — often just an overnight stay or even same-day discharge — reducing both cost and exposure to hospital-acquired infections. Internal organs experience less handling and manipulation, which means less post-operative adhesion formation and a quicker return of normal bowel function.
Common procedures performed laparoscopically
Laparoscopy is now the standard approach for a wide variety of abdominal and pelvic surgeries. The most commonly performed laparoscopic procedures include cholecystectomy (gallbladder removal), appendectomy (removal of the appendix), hernia repair (inguinal and ventral), colectomy (partial or full removal of the colon), bariatric surgeries such as sleeve gastrectomy and gastric bypass, hysterectomy, treatment of endometriosis, ovarian cyst removal, and diagnostic laparoscopy for unexplained abdominal pain or infertility investigation.
Increasingly, surgeons are also performing more complex procedures laparoscopically — including certain liver resections, pancreatic surgeries, and colorectal cancer operations — as technology and surgical expertise continue to advance.
What to expect: before, during, and after
In the days before surgery, your surgeon will advise you to fast for at least six to eight hours, stop certain medications such as blood thinners, and undergo pre-operative blood tests and imaging. You will meet your anaesthetist, who will review your medical history.
During the procedure, you will be completely unaware, lying under general anaesthesia. The surgery typically lasts between one and three hours depending on the complexity. Afterwards, you will be moved to a recovery room where nursing staff monitor your vital signs, pain levels, and nausea as the anaesthesia wears off.
At home, mild shoulder tip pain is common for the first 24–48 hours — this is a referred sensation from the CO₂ gas pressing on the diaphragm and resolves on its own. Small wounds should be kept dry for 48 hours. Most patients find paracetamol and ibuprofen sufficient for pain management, with stronger prescriptions available if needed.
Who is a good candidate?
Most healthy adults are suitable candidates for laparoscopic surgery. However, it may not be the preferred approach for patients who have had extensive previous abdominal surgeries that resulted in dense scar tissue (adhesions), those who are extremely obese, or in emergency situations where speed is critical. Your surgeon will assess your complete medical history, imaging results, and anatomy before recommending the best surgical approach for your individual case.
Risks and when to call your doctor
Like any surgical procedure, laparoscopy carries risks — though these are generally lower than with open surgery. Potential complications include bleeding, infection at the incision sites, unintended injury to surrounding organs such as the bowel or bladder, and reactions to anaesthesia. Conversion to open surgery mid-procedure is always possible if the laparoscopic approach becomes unsafe or technically unfeasible.
Contact your surgeon promptly if you experience fever above 38.5°C, increasing redness or discharge from wound sites, severe abdominal pain that is worsening, inability to pass gas or bowel movements beyond 48 hours, or difficulty breathing.
The future of laparoscopic surgery
Laparoscopic surgery continues to evolve rapidly. Robotic-assisted laparoscopy — led by systems such as the da Vinci Surgical System — gives surgeons enhanced 3D visualisation, a greater range of instrument motion, and improved precision for complex procedures. Single-incision laparoscopic surgery (SILS) performs entire operations through a single navel incision, leaving virtually no visible scar. Natural orifice transluminal endoscopic surgery (NOTES) — still in development — aims to operate entirely without external incisions. Artificial intelligence is beginning to assist in surgical navigation, tumour identification, and real-time decision support. The field is moving fast, and patients today benefit from a generation of innovation that has made surgery safer, less painful, and more effective than ever before.